“Boarding duration (in en ER) is a direct risk factor for developing delirium or severe agitation,” a research study found.
Article content
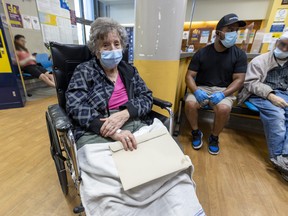
On Monday afternoon, the average length of what is known as emergency room boarding at Lakeshore General Hospital was nearly 30 hours. These patients on stretchers were all awaiting an inpatient bed. But beyond the grim statistic, what is the psychological impact of waiting this long?
Many, if not most, of the patients languishing on stretchers in the Lakeshore ER are in their 60s, 70s and 80s. Some are suffering from varying degrees of dementia. Yet they often remain stuck on stretchers for hours and hours. Again, what is the impact on their mental health?
Advertisement 2
Story continues below
Article content
A study published last month in the Journal of the American Medical Association attempted to answer that question. Researchers studied ER patients in hospitals in the Boston area from Jan. 1, 2018, to Dec. 31, 2022.
“The findings suggest that (emergency department) boarding duration is a direct risk factor for developing delirium or severe agitation during inpatient admission,” the researchers concluded. “Building on prior study results, we found this risk to be magnified in patients with dementia.”
But there’s a critical difference between the length of time Boston patients had endured and the scenario that’s been unfolding for years at the Lakeshore and other Montreal ERs. In Boston, the researchers found that those experiencing delirium waited an average of 206 minutes. That’s minutes.
By comparison in Montreal, some patients are boarded in ERs for up to five or six days, bereft of any privacy, sometimes going without meals, wearing flimsy hospital gowns that do not protect against bed sores. What is the impact of such boarding on their psychological health, as they are kept in corridors, sometimes placed in physical restraints, as a Quebec ombudsman’s report into the Lakeshore in Pointe-Claire discovered? No doubt it’s worse.
Article content
Advertisement 3
Story continues below
Article content

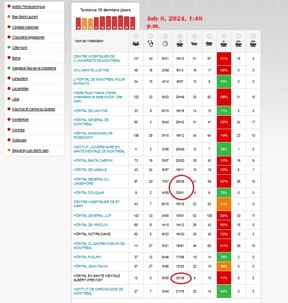
One could imagine that all this boarding might be even more distressing for mentally ill patients stuck in psychiatric ERs awaiting an inpatient bed. On Monday, the average length of stay on a stretcher in the ER of the Douglas Mental Health University Institute was nearly 31 hours. That’s hours, not minutes.
The Douglas in Verdun is the same psychiatric hospital where some patients were forced last year to lie for hours on mattresses strewn on the floor in an open corridor — a disturbing practice that Health Minister Christian Dubé ordered an end to only after The Gazette reported it.

For the record, the Montreal ER with the longest average wait on a stretcher on Monday was at the Albert-Prévost Mental Health Hospital in north-end Ahuntsic-Cartierville. The wait there was 32 hours and 36 minutes. For psychiatric patients.
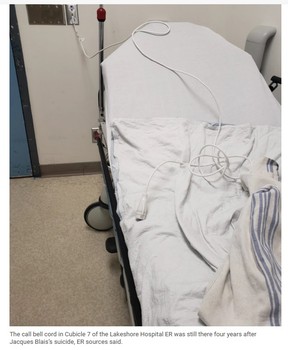
To return to the saga of the Lakeshore, The Gazette last year documented six likely-preventable deaths in its under-resourced and over-crowded ER. One death involved the suicide of a psychiatric patient. That patient, a retired provincial police officer, was known to the ER staff to be suicidal, yet he was left in a corridor on a stretcher for 14 hours, unsupervised, before he took his life in one of the cubicles. He used the cord of a call bell — which patients press on a button to gain the attention of a nurse — to hang himself.
Obviously, none of this is the fault of dedicated ER staff — nurses, doctors and orderlies — who are working under impossible conditions every day, afflicted what is known as moral injury, being forced to tolerate what should never be tolerated. So yes, ER boarding does have a psychological impact on patients — and it’s likely far worse in Quebec than in the U.S.
Recommended from Editorial
Advertisement 4
Story continues below
Article content
Article content


Comments